Jump to:
10 Things That Make Dr. Shah Different
Hover over the face to explore procedures.
Hover over the face to explore procedures.

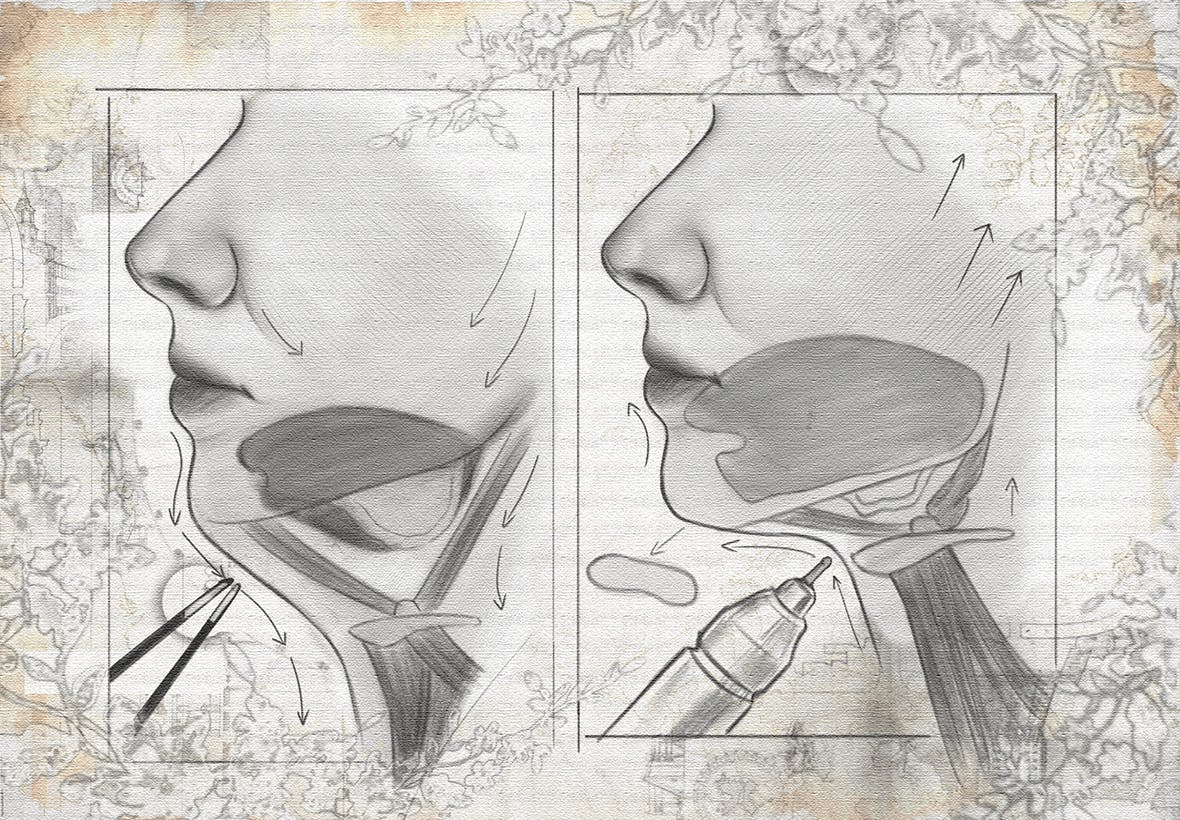
Deep neck contouring is one of the most technically demanding procedures in facial plastic surgery. Success hinges on a deep understanding of anatomy and the precision of the tools used in the procedure.
Dr. Shah authored the first scientific paper on ultrasonic neck reshaping, and was the first surgeon to apply ultrasonic dissection to deep neck contouring. His research shows utilizing ultrasonic instruments, which rely on precision, can offer safety advantages over traditional cautery devices, which rely on heat.
By operating at a lower, controlled temperature, ultrasonic dissection allows for more refined tissue sculpting, while minimizing disruption to surrounding nerves and salivary structures. The resulting outcome is a more predictable contouring, reduced risk of prolonged swelling, and a smoother recovery profile.
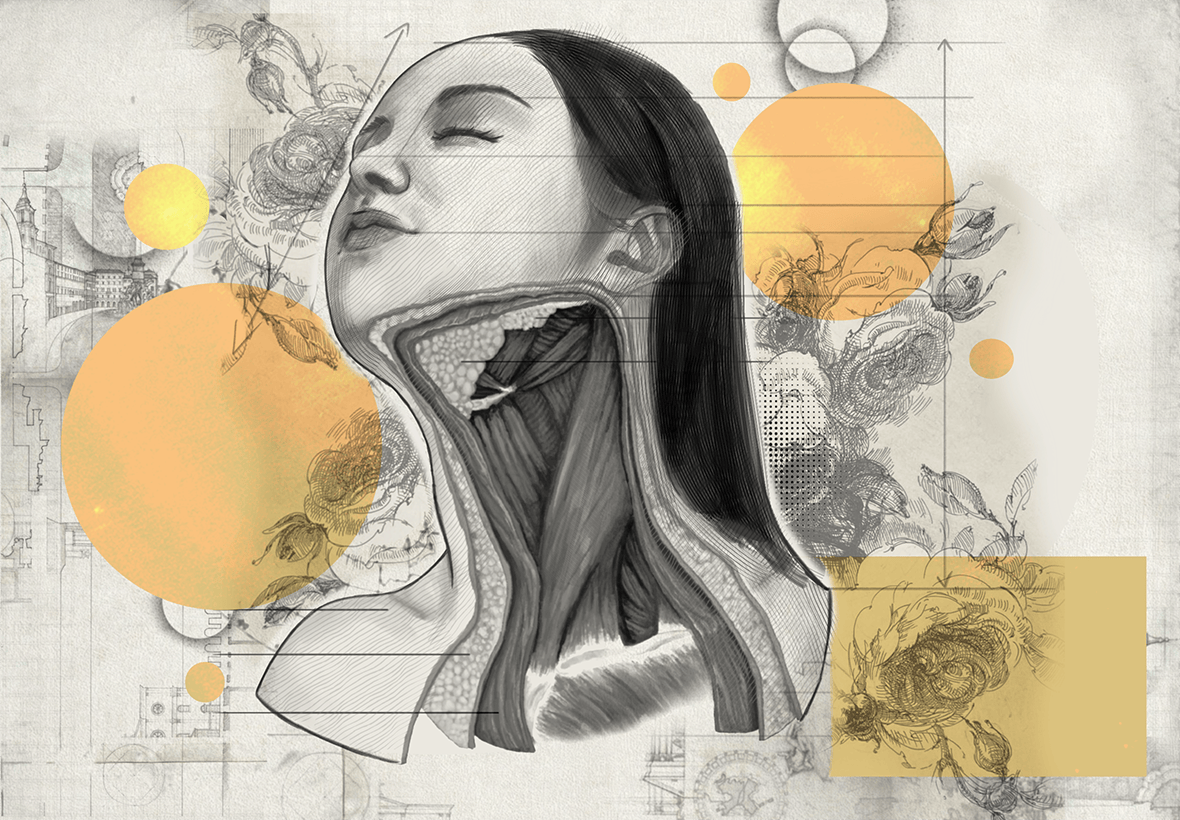
The neck is not a single layer, it is a complex, multi-layered structure. Many necklift procedures only address the neck's skin and superficial fat. More advanced techniques will extend deeper, but true transformation requires working through all five anatomical layers.
The deepest level of the neck comprises of the hyoid bone and its muscular attachments, which both influence the contour and function of the neck. As the hyoid descends with age, the jawline softens and neck loses definition.
By restoring structural support at this foundational layer, the neck can be reshaped in a more lasting and significant way.
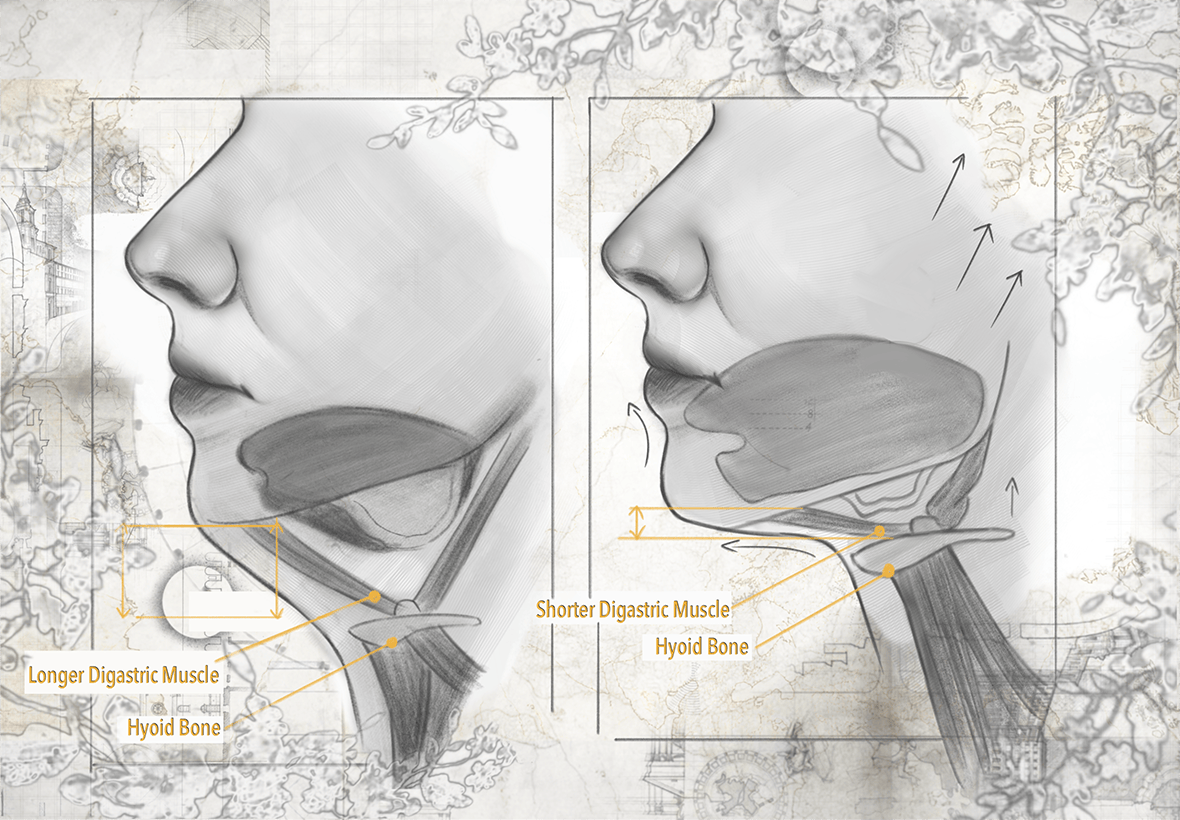
Beneath the visible layers of the neck is a deeper muscle, the digastric, which is often ignored by surgeons during a necklift, or resected during more "advanced" procedures. The two segments of the neck- the anterior and posterior- determine whether a neck looks long and elevated, or compressed and heavy.
Generally, the longer, more refined necks often feature a longer anterior digastric muscle. This creates a sharper jawline and accentuates the definition between the neck and the jawline. With age, this anterior segment will shorten, leading to a loss of definition.
While most approaches either ignore or resect this layer, Dr. Shah developed and published the first technique designed to restore and lengthen the anterior digastric using tissue from the posterior segment. Through this, he is able to elevate the hyoid bone, which anchors the neck's deeper architecture. This refinement produces a more durable contour and, in some cases, functional improvement including reduced snoring.
At the center of the neck's architecture sits a small, free-floating bone called the hyoid. If defines the angle of the jawline and the contour beneath the chin. As you age, the deeper tissues of your neck descend, and your strap muscles contract, which pulls the hyoid downward, softening your profile. Without addressing the positioning of the hyoid, the neck can't be transformed to its greatest potential.
Dr. Shah has published multiple landmark papers outlining advanced techniques which reposition and support the hyoid by working through the deeper muscles of the neck, rather than relying solely on skin and muscle tightening, restoring the neck and its foundation.
Advanced 5D computer modeling is used to evaluate airway dynamics and hyoid position. This allows for more precise surgical planning, predicting how structural adjustments will influence both contour and breathing function. When the hyoid is elevated and stabilized, the jawline is sharpened, the neck is elongated, and the result is more durable and longer-lasting.
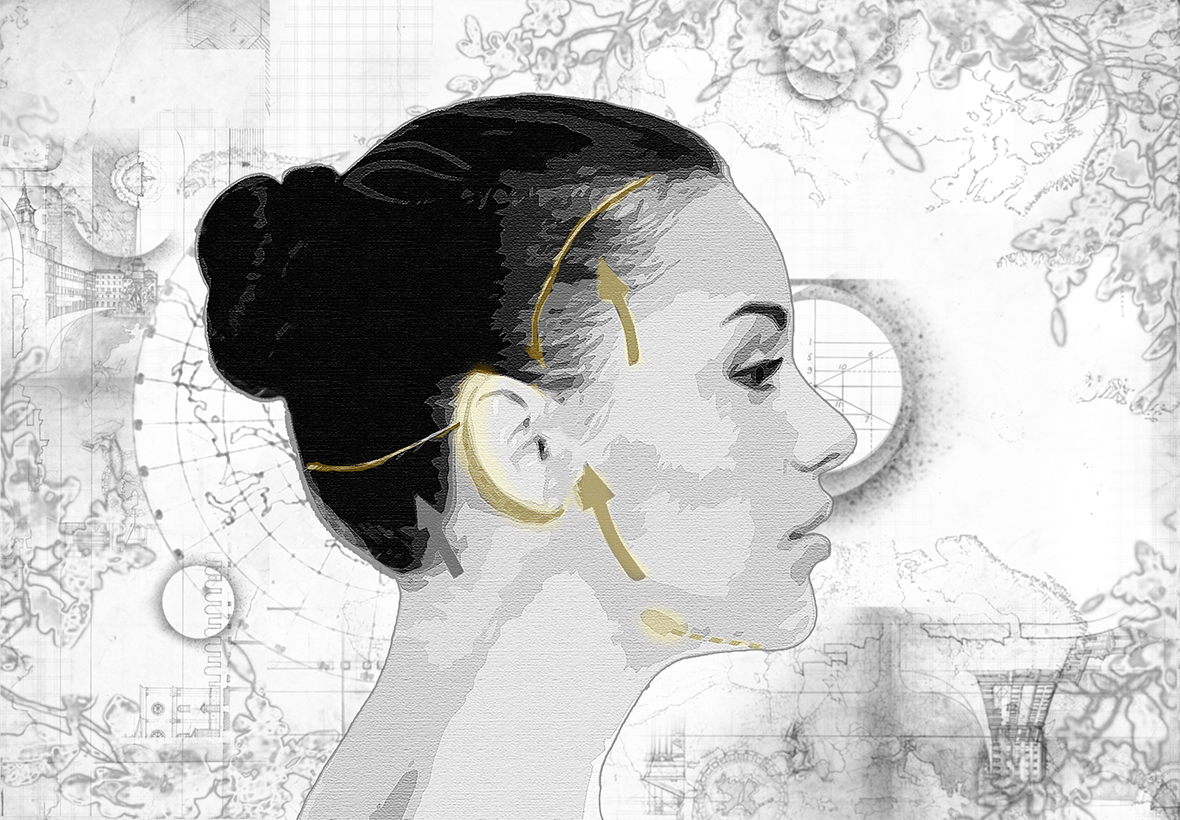
One of the most common signs of a traditional neck lift is a long incision extending into the nape of the neck. While this technique is effective for skin draping, it can limit hairstyles, risk hairline thinning, and leave a visible scar in a high-mobility area.
In the majority of his procedures, Dr. Shah works to avoid the nape entirely. Instead, the incision remains hidden within the natural crease behind the ear. This is possible because the lift does not rely on pulling skin backwards. Instead, by addressing deeper structures, the neck is reshaped internally, and the skin drapes naturally without unnecessary tension.
This means there is no visible posterior scarring, no hairline distortion, and a more natural result.
A facelift works by releasing the facial tissue from its original location and suspending it to a new location to create the desired facial shape. But where is the best location to suspend that tissue from? Often, surgeons will anchor this tissue from mobile structures in the face. This, however, inevitably leads to the lift weakening over time. Suspension requires stability. Like how a climber secures their lines to solid rock instead of a bending branch, facial tissue needs to be fixed to immovable anatomical points to ensure durability.
In his research, Dr. Shah identified key anchoring points capable of withstanding larger force without experiencing stretch relaxation. By securing the tissue to these stable points, tension is distributed more evenly across the face, and longevity is enhanced.
In a facelift, the biggest question is not how much to lift, but what to lift. The platysma, while commonly associated with the neck, also has a significant facial impact. In your youth, the muscle can extend to over half of the lower face, which helps with jawline definition and support. With age, the platysma gradually descends, leading the mid and lower face to descend in turn.
Rather than just lifting soft tissue layers, Dr. Shah focuses on restoring and repositioning the descended muscle, which creates a more natural lifted appearance. The process of lifting what is no longer on the face instead of tightening what still is on the face is what creates that balanced and natural result.


Upper blepharoplasties are performed to refresh the appearance of the eyes, but long-term success frequently depends on evaluating the brow as well. The brow and eyelid are closely connected both anatomically and neurologically, meaning changes to one structure can influence the other.
Research has shown that drooping of the eyelid can affect brow position, and simple biomechanics also play a role. When excess skin is removed from the upper eyelid, some downward tension can be transmitted to the brow. In certain cases, removing only a few millimeters of eyelid skin may subtly lower the brow over time.
For this reason, Dr. Shah will evaluate whether brow stabilization or a brow lift should accompany upper eyelid surgery. The goal is not always to raise the brow dramatically, but to support its position and create a stable foundation for eyelid rejuvenation.
By addressing both the eyelid and brow when appropriate, patients often achieve more balanced, natural-looking, and longer-lasting results.

Everyone knows that surgical drains are a pain. Drains, which are small plastic tubes placed beneath the skin to remove fluid or blood that can accumulate after surgery, are commonly utilized alongside tight compression wrapping after surgery. While they're useful for reducing the risk of hematoma or seroma, they're inconvenient, bulky, and often highly uncomfortable during the early recovery period.
Nowadays, however, drains aren't always necessary. Dr. Shah's approach to facelift recovery focuses on preventing fluid accumulation in the first place, rather than relying on tubes to remove it after it forms.
This is accomplished through the use of advanced, multi-layer fibrin sealants strategically placed within the deeper layers of the face and neck. These are biologic tissue adhesives that mimic the body's natural clotting mechanisms. This technique reduces the potential space where fluid can collect, controls microvascular bleeding, and allows the body to begin healing quicker without the disruption of fluid accumulation between layers. In all, this reduces swelling, bruising, and improves overall patient comfort compared to traditional drain-based approaches.
This method also eliminates the need for the tight wrapping. The excessive compression can collapse the delicate vessels that fluid drains through, slowing drainage rather than improving it. Heavy wrapping can also impair venous return, which can lead to congestion, throbbing, and increased bruising. The taping approach supports natural lymphatic direction, maintains venous patency, reduces pressure-related discomfort, and minimizes rebound swelling.
Surgery is a major metabolic event. Your body has to rapidly produce collagen, repair tissues, and restore vascular integrity. Without appropriate nutritional support, the healing process is often slower and less efficient. As such, Dr. Shah places all of his surgical patients on a structured nutritional plan two weeks prior to surgery: one gram of protein per pound of body weight daily.
Protein provides the essential building blocks needed for the healing process, and inadequate intake can compromise tissue strength and prolong the recovery process. This intake helps maintain positive nitrogen balance, support collagen synthesis, reduce edema, and prevent muscle breakdown.
In addition to optimizing protein intake, targeted supplements can also support healing. Key supplements include Amino acids such as arginine and glutamine, which aid in surgical stress, Vitamin C, Zinc, and Copper, which assist in collagen formation and cross-linking, and various nutrients that reduce inflammation without increasing the risk of bleeding.
When nutrition and supplementation is prioritized before surgery, patients often see more predictable healing, improved scar quality, reduced fatigue, and earlier return to normal activities.

Historically, patients recovering from facial surgery are advised to use ice to control swelling. Though cooling is beneficial, traditional ice packs are inconsistent and excessively cold, which can interfere with normal healing. Dr. Shah has found utilizing Hilotherapy- a controlled cooling system- offers consistent temperature control, even cooling distribution across the face and neck, and greater comfort during the recovery period.
The Hilotherapy system uses a contoured facial mask that circulates cooled water evenly across the face. Unlike ice packs, which have to be frequently replaced, the Hilotherapy system can maintain stable cooling for several hours at a time, allowing for consistent temperature regulation, even distribution of cooling across the face and neck, and greater comfort during the early recovery period, which helps support the body's natural healing response after surgery.
Hilotherapy maintains a precise therapeutic temperature between approximately 15–18ºC (59–64ºF), which is far superior to ice's temperature of 0ºC (32ºF), which is colder than what healing tissue requires. With ice, lymphatic drainage can slow, bruising can increase, and tissue repair slows. Hilotherapy helps reduce inflammation and discomfort, while allowing the body's natural healing processes to continue.
Red light therapy is a treatment that uses specific wavelengths of light to stimulate healing and improve the appearance of the skin. It has been shown to be effective in a variety of conditions, including acne, rosacea, and eczema, and it may also be beneficial for helping a surgery patient heal, in ways such as:
Hyperbaric Oxygen Therapy, or HBOT, can be utilized to support post-surgical healing. Through placing the patient into a pressurized chamber and allowing them to breathe pure oxygen, the body is delivered higher levels of oxygen than it would otherwise receive normally. As oxygen plays a critical role in wound healing, collagen production, and the formation of new blood vessels, HBOT's pressurized oxygen flow can offer assistance to the body during the earlier phases of surgical recovery.
In some cases, HBOT can also assist in reducing inflammation and supporting recovery in patients who are experiencing delayed healing or complications. While it is not necessary for every surgical patient, it can be a valuable tool in a surgeon's recovery arsenal.
