
Use Of Intradermal Botulinium Toxin To Reduce Sebum Production And Facial Pore Size
Anil R. Shah, MD
200 West Superior St., Suite 200
Chicago, IL 60654
[email protected]
Objective: Review the safety profile and subjective efficacy of intradermal botulinium toxin in facial pore size and sebum production
Design: Retrospective Analysis
Results: 20 consecutive patients with a single application of intradermal botulinum toxin were examined. 17/20 patients noted improvement in sebum production and 17/ 20 noted decrease in pores size at one month after injection. 17/20 patients were satisfied with the procedure. No complications were observed.
Conclusion: Preliminary data suggests that intradermal botulinum toxin may play a role in decreasing sebum production. Further quantitive study may be necessary to determine effects of intradermal botulinum toxin on pore size.
Keywords: Botulinum toxin, pore reduction, sebum, hyperhydrosis, sweat,
Facial pore size and excessive sebum production are notoriously difficult skin conditions to treat. Numerous techniques have been described with limited results or significant drawbacks. A variety of skin resurfacing modalities have been described, but results have been mixed and inconsistent. One potential reason for this limitation is that the location of the sebaceous gland is in the deeper portion of the dermis, a difficult area to reach by resurfacing modalities.
Deeper resurfacing techniques can lead to hyper and hypopigmentation, especially in Fitzpatrick IV and above patients, long recovery periods and permanent scarring. Accutane’s (Roche Pharmaceuticals, Nutley, NJ), isotrentinoin, exact method of working is currently unknown, but it theoretically decreases sebum production. (1) However, one of the main drawbacks of accutane therapy is serious systemic side effects including liver dysfunction, mucosal bleeding, and cardiac disease. In addition, several studies have suggested a possible link between Accutane and depression, suicide, anxiety, and aggressive behavior. (2-6)
The use of intradermal botulinium toxin remains a relatively new technique. No reports in the literature describe its effects on sebum production and pore size. The author (ARS) first noticed that Botulinum toxin’s effects on the skin after injection along the procerus to treat “bunny lines”. Patients reported improvement in skin quality and less skin shininess. Further investigation lead to isolated reports from Southeast Asia of physicians using intradermal botox as a mechanism of treating enlarged pores and providing a “mini lift”.
Botulinum toxin has been employed in a variety of treatment throughout the body as an alternative to systemic therapy. In “sphincter therapy”, botulinum toxin works on a targeted, local level, rather than a macroscopic level. (7) It has the distinct advantage of limited systemic side effects. Traditionally, Botulinum toxin has been embraced recently for its effects on relaxation of voluntary skeletal muscles. However, Botulinum toxin’s primary modality of blocking the neurotransmitter acetylecholine has led to a variety of novel applications including effecting receptors.
The purported mechanism of action of botulinum pore reduction can be postulated based on its known neuromodulatory effects. Erector pili muscle are stimulated on the sympathetic/ parasympathetic level. The parasympathetic system works on a local level while the sympathetic system effects receptors from a distance by neuroganglions. Botulinum toxin acts on a local level blocking the parasympathetic response and leading to an over all increase in the sympathetic response.
Recently the muscarnic receptor has been studied in sebum production, noting that acetylcholine is responsible for sebum production. (8) Botulinum toxin can theoretically block this receptor on a local level.
Acetycholine plays a significant role in the regulatory function of skin processes such as kertioncyte differentiation, sebum production, microcirculation, and barrier protection. (9) Excess acetylcholine production has been demonstrated to occur in skin disorders such as vitiligo. Botox (Botulinum toxin, Subunit A) is a highly concentrated peptide which acts on blocking acetylcholine at the x receptor. Initially Botulinum toxin was utilized for distinct skeletal muscles at the x receptor including. dynamic wrinkles, correction of spasmotic disorders, Recently, its role has expanded to include broader applications including treatment of hyperhydrosis.
The author theorizes that intradermal injection of botulinum toxin may decrease sebum production, pore size, in addition to known effects on hyperhydrosis. No current study has examined the use of intradermal botulinum toxin in sebum production and pore size.
Methods
A retrospective chart review of 20 consecutive patients who received a single application of intradermal botulinum toxin for the purpose of excessively large pores or excessive sebum production in the private practice of the senior author (ARS). Patients were excluded from this study who had used accutane in the past, or had LASER treatment, IPL, or chemical peel in the effected areas. Patients were instructed to use noncomodogenic makeup and skin products after therapy. All patients were seen in the office at a minimum of two months post procedure. Patients were informed prior to treatment this was a non-FDA use of botulinum toxin.
Chart review was examined to determine if any sequlae were found and patients comments on the procedure.
All patients were seen at one week and one month after administration of intradermal botulinum toxin.
Skin was evaluated without makeup and previous treatments were written down. High quality photographic stills were taken with a 100 mm MacroLens Canon (USB 2.5) with a Canon 20D DSLR on each patient before therapy and one month immediately after treatment.
Technique
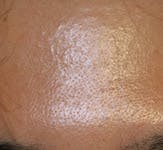
Before
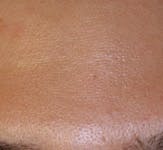
After
Informed consent of the “off label” use of Botulinum toxin was performed prior to each procedure. Potential risks of the procedure were mentioned including facial muscle paresis and excessive bruising and swelling.
The author (ARS) has made the following observations about the technical aspects of intradermal botulinum therapy. The use of intradermal Botulinum toxin is very technique sensitive. The appropriate layer the toxin must be injected in is the dermis. Placement of the botulinum toxin too superficially will lead to ineffectiveness, while placement too deep can lead to unintended facial weakness, especially when used over the medial cheeks.
Although topical anesthesia can mitigate discomfort with this technique, the author prefers to avoid topical anesthesia. Standarized botulinum toxin injection is typically painless. However, intradermal botox is injected into several areas where conventional botox therapy is not used, including the nose and medial cheek. These areas are much more sensitive than the upper facial one third. In addition the subepidermal nerve plexus and epidermis nerves make the more superficial tissues much more sensitive than deeper tissues.
The author recommends a dilution of 5 cc of Bacteriostatic saline per 100 units of Botulinum toxin based on his limited clinical observations. He has found more diluted concentrations (10cc) have less length in duration of effects. Supraconcentrated doses, (1 cc dilutions) do not seem to provide any additional potency to the treatment and require more needle sticks due to less diffusion out amongst the tissues.
The author (ARS) prefers the use of 30 gauge or smaller needles to limit bruising and pain with injection. The needle is placed at a 75 degree angle to the contact area of the skin, facilitating placement of Botulinum in the dermis. When injecting into the skin, the injector may notice some of the solution exiting neighboring pores, an indication that the injector is in an appropriate location. In Fitzpatrick I and II skin types, the skin may blanch when injected into the dermis.
Most patients note a “tingling” sensation which persists for several days after treatment and notice tightening of the injected areas beginning as early as one day to a week.
Results
Chart review demonstrates that all patients were being treated for oily skin complexion, with 15/20 patients also complaining about large pores and 15/20 patients complaining about acne prone skin.
No complications were noted including facial weakness. 6/20 patients noticed minor postinjection erythema along which persisted along the medial cheek and nose for approximately 72 hours.
At the one month follow up period, 17/20 patients noted improvement in skin oilness after one treatment of intradermal botulinum toxin. 17/20 patients described improved facial pores.
Discussion
Botox has revolutionized the treatment of facial rhytids. Its role in facial pore size and sebum has not been well studied. This preliminary report suggests that intradermal botox can be injected safely in the area of the forehead, medial cheek, and nose without complication. In addition, one treatment of intradermal botulinum toxin subjectively reduced skin oiliness in 17/20 patients and pore size in 17/20 patients. Further treatments with intradermal botulinum toxin may reduce skin oil production in patients not affected by this therapy.
A major weakness of this study is that objective measures were not taken. Further study may help elucidate the effectiveness of intradermal botulinum toxin and degree of improvement with this therapy.
The author (ARS) has previously written about standardization in dermatologic photographs. Although photographs were taken in a standardized method, determining the degree of sebum production with a photograph is difficult. Pore size is also difficult to quantify based on photography. Allowing the patients to subjectively determine if there was improvement was used to provide a simple determination of efficacy and allow for more formalized objective studies to take place at a later date.
Botox’s role in targeted therapy without systemic consequences may eventually make it an alternative to accutane in the treatment of oily skin and acne prone skin. Additionally, applications of intradermal botox theoretically could prophylatically prevent the creation of enlarged pores. Patients with shiny skin have difficulty with excess facial sebum. Facial blotting may in fact encourage more sebum production. Treating the root cause of excess sebum may lead to more innovative approaches to the oily complexion.
A potential complications from this therapy is facial paresis, especially because of treating muscles along the face/ zygomaticus major/ minor perioral muscle. Controlling the depth of injection is critical in order to maximize therapeautic efficacy of the treatment while preventing untoward sequlae. Although meso-techniques for injecting the dermis exist, however, skin thickness varies significantly from patient to patient and the author prefers manual injection for precision and individualized treatment.
The injection is limited to the T zone of the face including the forehead, glabella, nose, and medial cheek. Coincidentally, these are the most common areas of complaint of acne and shiny skin. The author does not inject along the mental region due to the superficial location of the facial nerve in this region, especially since the only location where the facial nerve is superficial to the muscle is at the mentalis, levator, buccinator. The malar fat pad provides a natural barrier between the underlying facial muscles, making injection along the medial cheek safe. Patients with a paucity of fat along the malar regions should be injected cautiously.
Some patients noted that the procedure was uncomfortable and that a small amount of erythema can last for up to 48 hours. The author has used topical anesthetics in the past prior to injection but prefers to not use them for several reasons. First of all, when botulinum toxin is injected in the correct layer, patients often describe a tingling sensation. The use of topical anesthetics can mimic this response and make it difficult to determine the source of the tingling. The author discourages the use of alcohol pads after injection to avoid any breakdown of the botulinum toxin protein and prefers normal saline.
It can not be determined whether or not Botulinum toxin actually shrinks the pore. It is unlikely that an overly stretched pore will reduce in size, even with arector pili muscle stimulation. Some of the high quality photographic stills noted improved sebum production and oilness to the skin. However, demonstration of pore size reduction by macro photography is very difficult. A future study quantifying pore size with a quantitative measures may be necessary to determine the degree pore size is impacted. Patients note a tighter feeling to the skin which may be a result of decreased sebum production.
The mechanism of affecting the arector pili muscle is not known. The author (ARS) theorizes that an interplay on the sympathetic / parasympathetic system may effect muscular tone. Normally the sympathetic system stimulates the erector pili muscle causing pore contraction. However, the sympathetic system receptor is located distally from the muscle. The parasympathetic system is located near the muscle. The parasympathetic system relaxes the arector pili muscle. By selectively blocking the parasympathetic system, the sympathetic system theoretically will exert a relatively increased force on the arector pili muscle, leading to contracture of the muscle and decrease in pore size.
The sebum production is influenced by the muscarnic receptor (acetylcholine). Similarly, botulinum toxin will effect this receptor and cause a relative decrease in sebum production.
The use of botulinium toxin continues to revolutionize the medical field with new applications. Botulinum toxin represents a targeted therapy with minimal systemic effects. Although this study may demonstrate a role of botulinium toxin in reducing sebum and pore size, further studies are necessary with more objective measures.
References
- Zouboulis CC. Isotretinoin revisited: pluripotent effects on human sebaceous gland cells. J Invest Dermatology. Oct 2006; 126 (10): 2154-6.
- O’Donnell J. Overview of existing research and information linking isotretinoin (accutane), depression, psychosis, and suicide. Am J Ther 2003;10(2):148-59. PMID 12629595
- Bremner JD. Does isotretinoin cause depression and suicide? Psychopharmacol Bull 2003;37(1):64-78. PMID 14561949
- Wysowski DK, Pitts M, Beitz J. An analysis of reports of depression and suicide in patients treated with isotretinoin. J Am Acad Dermatol 2001;45(4):515-9. PMID 11568740
- Ng CH, Schweitzer I. The association between depression and isotretinoin use in acne. Aust N Z J Psychiatry 2003;37(1):78-84. PMID 12534661
- Hull PR, D’Arcy C. Isotretinoin use and subsequent depression and suicide: presenting the evidence. Am J Clin Dermatol 2003;4(7):493-505. PMID 12814338
- Franco I, Landau-Dyer L, Isom-Batz G, Collett T, et al. The use of botulinum toxin A injection for the management of external sphincter dyssynergia in neurologically normal children.
- Kurzen H, Schallreuter KU. Novel aspects in cutaneous biology of acetylcholine synthesis and acetylcholine receptors. Exp Dermatol. 2004;13 Suppl 4:27-30.
- Kurzen H, Wessler I, Kirkpatrick CJ, Kawashima K, et al. The non-neuronal cholinergic system of human skin. Horm Metab Res. 2007 39(2): 125-35.
Disclosure:
No conflicts of interest including financial or otherwise.


